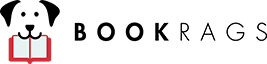Residual abscess is the name given to an abscess that makes its appearance months, or even years, after the apparent cure of tuberculous disease—as, for example, in the hip-joint or spine. It is called residual because it has its origin in the remains of the original disease.
[Illustration: FIG. 34.—Tuberculous Abscess in right lumbar region in a woman aged thirty.]
#Diagnosis.#—A cold abscess is to be diagnosed from a syphilitic gumma, a cyst, and from lipoma and other soft tumours. The differential diagnosis of these affections will be considered later; it is often made easier by recognising the presence of a lesion that is likely to cause a cold abscess, such as tuberculous disease of the spine or of the sacro-iliac joint. When it is about to burst externally, it may be difficult to distinguish a tuberculous abscess from one due to infection with pyogenic organisms. Even when the abscess is opened, the appearances of the pus may not supply the desired information, and it may be necessary to submit it to bacteriological examination. When the pus is found to be sterile, it is usually safe to assume that the condition is tuberculous, as in other forms of suppuration the causative organisms can usually be recognised. Experimental inoculation will establish a definite diagnosis, but it implies a delay of two to three weeks.
#Treatment.#—The tuberculous abscess may recede and disappear under general treatment. Many surgeons advise that so long as the abscess is quiescent it should be left alone. All agree, however, that if it shows a tendency to spread, to increase in size, or to approach the skin or a mucous membrane, something should be done to avoid the danger of its bursting and becoming infected with pyogenic organisms. Simple evacuation of the abscess by a hollow needle may suffice, or bismuth or iodoform may be introduced after withdrawal of the contents.